Research: How to help overcome vaccine hesitancy for Black Americans
With data showing that communities of color are more likely to be skeptical of messages encourage vaccine adoption—despite adverse outcomes from the COVID-19 pandemic—here’s how to push back.

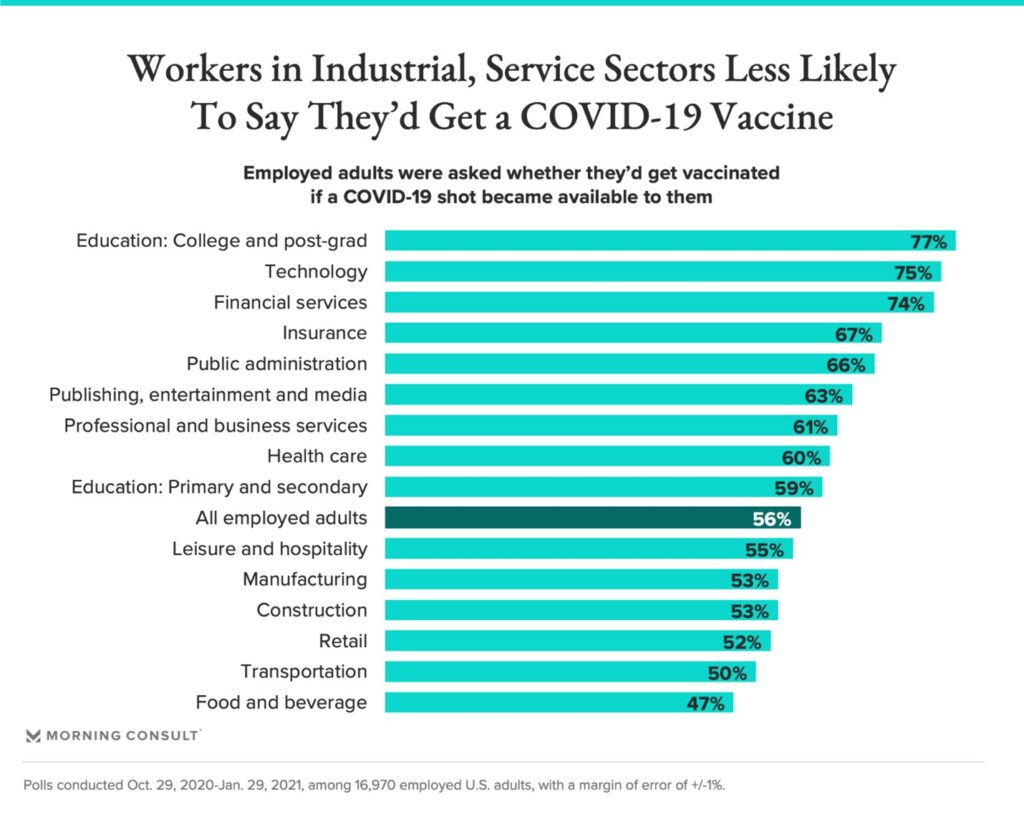
For organizations and wellness pros looking to amplify vaccine messaging, the increase in vaccine skepticism in the U.S. is a major concern. In data from Morning Consult, a little more than half (56%) of working adults said they would readily take a COVID-19 vaccine if offered one.
Black Americans have been more hesitant when it comes to vaccines, for a variety of reasons from poor health care options in their communities to historic injustices and mistreatment at the hands of health care companies and government agencies.
What does the research suggest can be done to help drive vaccine adoption in these communities? Here are some recommendations from researchers.
1. Don’t ignore mental health.
Higher rates of depression could be linked to a reduced rate in vaccine adoption, argues one paper published in BioMed Research International. The paper, titled “Influenza Vaccination among Underserved African-American Older Adults” makes the connection between instances of depression in patients leading to fewer attempts to receive care and treatment.
“We documented that among our sample of underserved African-American older adults, participants with a higher number of depression symptoms were less likely to be vaccinated,” the paper says, noting that depression is more chronic and disabling, as well as less likely to be treated for African Americans.
Therefore, mental health services and offerings are a vital part of addressing vaccine adoption, especially for populations already facing disparate health care outcomes.
2. Double down on transparency.
In the article “A Tale of Two Crises: Addressing Covid-19 Vaccine Hesitancy as Promoting Racial Justice,” published on the HEC Forum, author Laurne Bunch offers a handful of recommendations for communicators looking to break through with underserved audiences like the Black community when it comes to vaccines.
Bunch argues that fears about how fast the vaccine was developed or mistrust of pharmaceutical companies in general can be counterbalanced by radical honesty. However, that doesn’t mean offering statements filled with scientific jargon.
“Releasing documents filled with scientific jargon is transparent in only a trivial sense,” Bunch writes. “To be transparent in a way that combats mistrust and suspicion of motives, those involved in vaccine development and approval must craft their disclosures in such a way that non-expert audiences can readily understand their contents.”
Transparency also includes being open and honest about uncertainty, and explaining how the scientific method helps offer certainty over time. Bunch writes:
“Particularly in the context of politicization and suspicion about motives, it is imperative that this uncertainty be forthrightly acknowledged. Appropriate acknowledgements of uncertainty include: that previously undetected adverse reactions may occur after a vaccine has been approved; that sterilizing immunity is unlikely to occur; and that long-term efficacy will not immediately be known.”
3. Offer critical distance from pharmaceutical companies.
Messages about the safety of vaccine must come from someone other than the companies that stand to make huge profits from their latest drug—despite all their best intentions.
“Given the high levels of suspicion that Americans in general and Black Americans in particular have toward pharmaceutical companies (Jamison et al. 2019), we ought to ensure that communications about the efficacy, safety, and importance of vaccination are not coming from pharmaceutical companies,” Bunch writes.
However, she notes that some messages should come from the pharma companies, specifically updates and explanations about setbacks and reasons why a drug has failed to be developed on time.
4. Target your messages as specifically as you can.
In a paper titled “Black-white disparities in 2009 H1N1 vaccination among adults in the United States: A cautionary tale for the COVID-19 pandemic,” published in ScienceDirect, the authors argue that specific demographics are less likely to pursue a COVID-19 vaccine than others based on historic flu vaccine data.
Factors such as socioeconomic status and community health beliefs can all be factors that contribute to why a consumer doesn’t trust vaccines or pursue a vaccine. However, in broad strokes, the study identified white women as the most likely to get vaccinated, followed by white men, then Black men and Black women were the least likely.
The study reported that the strongest indicator of a vaccine adoption for H1N1, and therefore a COVID-19 vaccine now in the present day, was a recommendation from a personal health care provider or doctor.
The study also recommends specific action to address the inequality in outcomes and vaccine rates for communities of color. “Health campaigns designed to address the unique concerns of various racial and ethnic minorities could be a crucial component in reducing health inequalities,” it says.
5. Consider tactics to encourage “intellectual humility.”
People who have “intellectual humility,” according to social scientists, are more willing to be challenged on their beliefs and intake new information or learn new data. The trait is highly predictive of a willingness to vaccinate, according to the paper, “A little shot of humility: Intellectual humility predicts vaccination attitudes and intention to vaccinate against COVID‐19” published in the Journal of Applied Social Psychology.
The reason to focus on intellectual humility is because of research which shows that the trait can be encouraged in an audience, write the paper’s authors: “The particular benefit of humility is that there are known experimental interventions to increase its levels via writing prompts, gratitude, or experiences of awe.”
For communicators looking to encourage audiences to change their views on COVID-19 vaccine adoption, these kinds of tools and tactics could be highly valuable.